Asthma education: clear, practical steps to breathe easier
Nearly 1 in 13 people have asthma, yet many flare-ups happen because simple skills are missing. This short guide gives concrete steps you can use today: how to handle inhalers, build an action plan, cut triggers, and know when to get urgent help.
Know the basics and your pattern
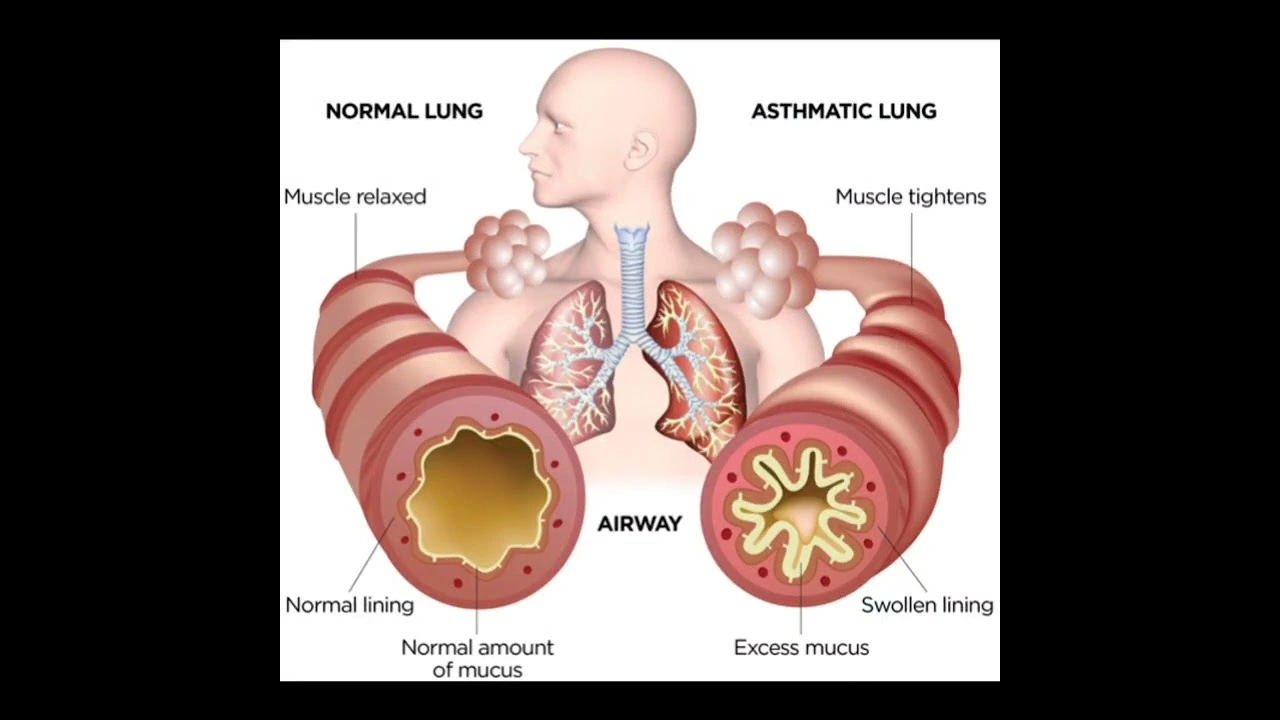
Asthma causes inflamed, narrow airways that make breathing hard. Symptoms include wheeze, cough, chest tightness, or breathlessness. Pay attention to when symptoms show up: at night, during exercise, after exposure to pets or dust, or when you get a cold. Write these patterns down — they help your clinician choose the right treatment.
Keep a simple symptom diary for two weeks: note time of day, what you were doing, and how you felt. That short habit gives a clear picture of triggers and control.
Inhaler technique, step by step
Wrong inhaler use cuts drug effect by a lot. For pressurised (pMDI) inhalers use a spacer if possible: shake the inhaler, put one puff into the spacer, breathe out fully, seal your lips around the spacer mouthpiece, breathe in slowly and deeply, hold your breath for about five to ten seconds, then breathe out. For dry powder inhalers breathe out gently, place the mouthpiece to your lips, inhale fast and deep, then hold your breath. Rinse your mouth after steroid inhalers to reduce the chance of thrush.
Ask a nurse or pharmacist to watch you use your inhaler. A quick check and a correction can make medicines work much better.
Carry your reliever inhaler (short-acting bronchodilator) at all times. Use it at the first sign of tightness. If symptoms need more puffs or persist, follow your action plan.
Preventer inhalers (inhaled corticosteroids) lower inflammation over weeks and reduce flares. Combination inhalers pair a steroid with a long-acting bronchodilator for ongoing control. Montelukast is an oral option often used when allergies play a role; check side effects and discuss mood changes with a clinician if they occur.
For people with hard-to-control asthma there are specialist options like biologic treatments. Ask your doctor if your symptoms aren’t improving despite proper inhaler use and regular reviews.
Use a peak flow meter at the same time each day to track lung function. Compare readings to your personal best and follow green, yellow, red zone rules in your action plan. If peak flow drops significantly, act early.
Reduce triggers: keep the home smoke-free, wash bedding weekly, use allergen covers, limit strong sprays, and manage pets so they stay out of bedrooms. Warm up before exercise and have your reliever handy for exercise-induced symptoms.
Get urgent help if you can’t speak in full sentences, your lips or face turn blue, you become drowsy, or the reliever does not ease breathing quickly. Regularly review your plan with a clinician and keep a copy at home, work, and school. Practical, repeated checks of technique and triggers are the most reliable way to cut attacks and feel safer every day.
In my recent exploration around asthma treatment, I've discovered that combining Montelukast with proper asthma education can be incredibly effective. Montelukast, a medication used to control and prevent symptoms caused by asthma, works even better when combined with an understanding of the disease. By learning about asthma triggers, signs of an attack, and proper use of medication, patients can manage their condition more effectively. It seems that knowledge really is power when it comes to controlling asthma. So, folks, remember to educate yourselves while taking your medication for the best results.