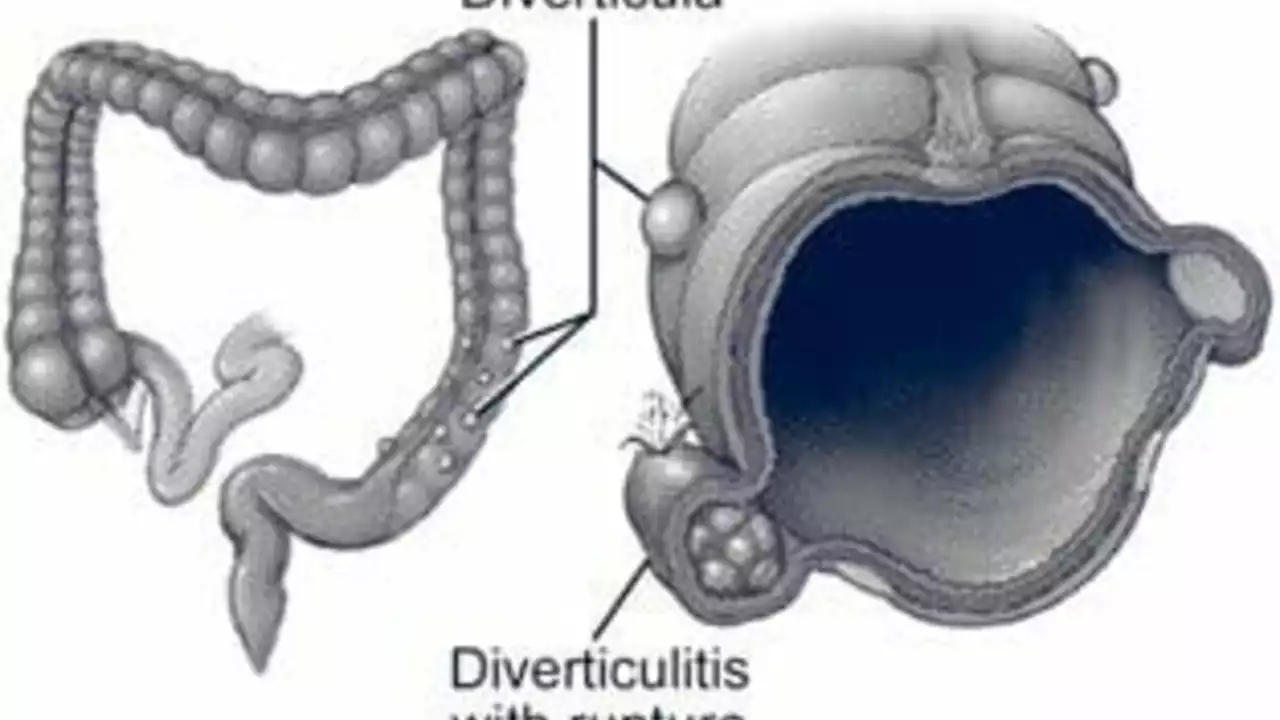
Diverticulitis management: clear steps for an attack and long-term care
Diverticulitis can feel sudden and scary: sharp lower belly pain, fever, and a change in bowel habits. Most people recover well if they act fast and follow simple rules. This page gives plain, useful advice on what to do right away, when to see a doctor, and smart habits that cut the chance of another episode.
What to do during an attack
If you get new lower abdominal pain with fever or nausea, call your doctor. For mild cases your doctor might suggest rest, a short liquid or low-fiber diet, and pain control at home. Use acetaminophen (paracetamol) for pain unless your clinician tells you otherwise. Try to avoid NSAIDs like ibuprofen and naproxen because they can raise complication risks for some people.
Decisions about antibiotics have changed: many uncomplicated cases are watched without antibiotics, while others still need them. Your doctor will decide based on exam, symptoms, and tests. If pain gets worse, you have a high fever, can't keep fluids down, see blood, or have fainting/lightheaded episodes, go to the emergency department. Those signs can mean an abscess, perforation, or sepsis—issues that need urgent care.
A CT scan is the usual test to confirm diverticulitis and check for complications like abscesses or blockages. If an abscess is found, it may need drainage or IV antibiotics. Severe complications sometimes require surgery right away.
Long-term steps to lower the risk
After recovery, focus on prevention. The strongest, simplest step is a high-fiber diet: aim for plenty of vegetables, fruit, whole grains, and legumes. If you find it hard to get enough fiber, a bulk-forming supplement like psyllium can help. Drink water and move regularly—walking 30 minutes most days supports regular bowel habits and lowers risk.
Old advice to avoid nuts, seeds, and popcorn is outdated. Recent evidence doesn’t show these foods cause attacks, so you usually don’t need to cut them out. Some research links high red-meat intake with more diverticulitis, so cutting back on processed and red meat is a reasonable choice.
Smoking increases risk; quitting helps. If you struggle with constipation, use gentle measures first—fiber, fluids, routine bathroom times—before laxatives. Probiotics may ease symptoms for some people, but they aren’t proven to prevent diverticulitis reliably.
Your doctor will likely recommend a colonoscopy a few weeks after recovery to rule out other causes such as polyps or colorectal cancer. Surgery to remove the affected colon part is now considered case-by-case—usually for repeated severe attacks or complications that don’t settle with medical care.
Keep a simple plan: know your warning signs, follow your clinician’s instructions during an attack, and make steady lifestyle changes afterward. That approach stops many repeat problems and keeps you living normally.
Alright folks, tackling Diverticulitis at work may seem like a daunting task, but hey, we've got this! First things first, keep those healthy snacks close at hand and don't skip meals - your tummy will thank you. Remember, hydration is key, so keep that water bottle filled and make frequent pit stops at the water cooler. Take short breaks to stretch and move about, because trust me, your gut loves a good walk! And finally, don't be shy about discussing your needs with your boss or HR - it's not like you're asking for a throne made of donuts!